ACL Reconstruction Rehabilitation Up To Date
Understanding the Critical Stages of ACL Reconstruction Rehabilitation
As someone who has undergone two ACL reconstruction surgeries (one in each knee), I have always been especially interested in the rehabilitation process after this surgery. That being said, as a clinician it’s extremely important for me to learn about the rehabilitation process that takes place immediately after any surgery. This period tends to be crucial for athletes who will eventually return to their sport, safely!
Importance of Early Weight Bearing After ACL Surgery
There is an abundant amount of research on rehabilitation after ACL reconstruction. This is because this is an injury commonly sustained by elite athletes and return to sport is usually significant (at times more than a year) which leads to other problems – from significant money loss (to the team and athlete), to psychological dysfunction (to the athlete due to increased stress levels as he/she misses sport).
A professional clinician like myself works to achieve the best outcome possible with athletes in two ways. One is education, including current research and literature. The second is experience, working with different individuals and constantly assessing and refining my approach.
Both my education and experience have lead me to four often overlooked key points that ensure that you as an athlete get back to sports as fast and as safely as possible after ACL reconstruction. These four points summarize what I’ve learned over the last decade as a physical therapist in regard to ACL reconstruction rehabilitation and sports performance.
1. Weight bearing is advised as soon as possible after the surgery. Unless otherwise stated by the surgeon, weight bearing, even with crutches, should start as soon as possible. This will lead to better knee mobility, reduced anterior knee pain, reduced loss of muscle mass and endurance, and an overall better rehabilitation outcome.
2. In many cases, bracing is not needed after surgery. Some surgeons are still wary of not using a knee brace in the early stages of rehabilitation to compensate for knee instability. However, most studies show that the use of a brace has major flows. These include increased pain, swelling, and inflammation and decreased range of motion, strength and neuromuscular control. Most importantly they have not been shown to lead to an increase in knee instability.
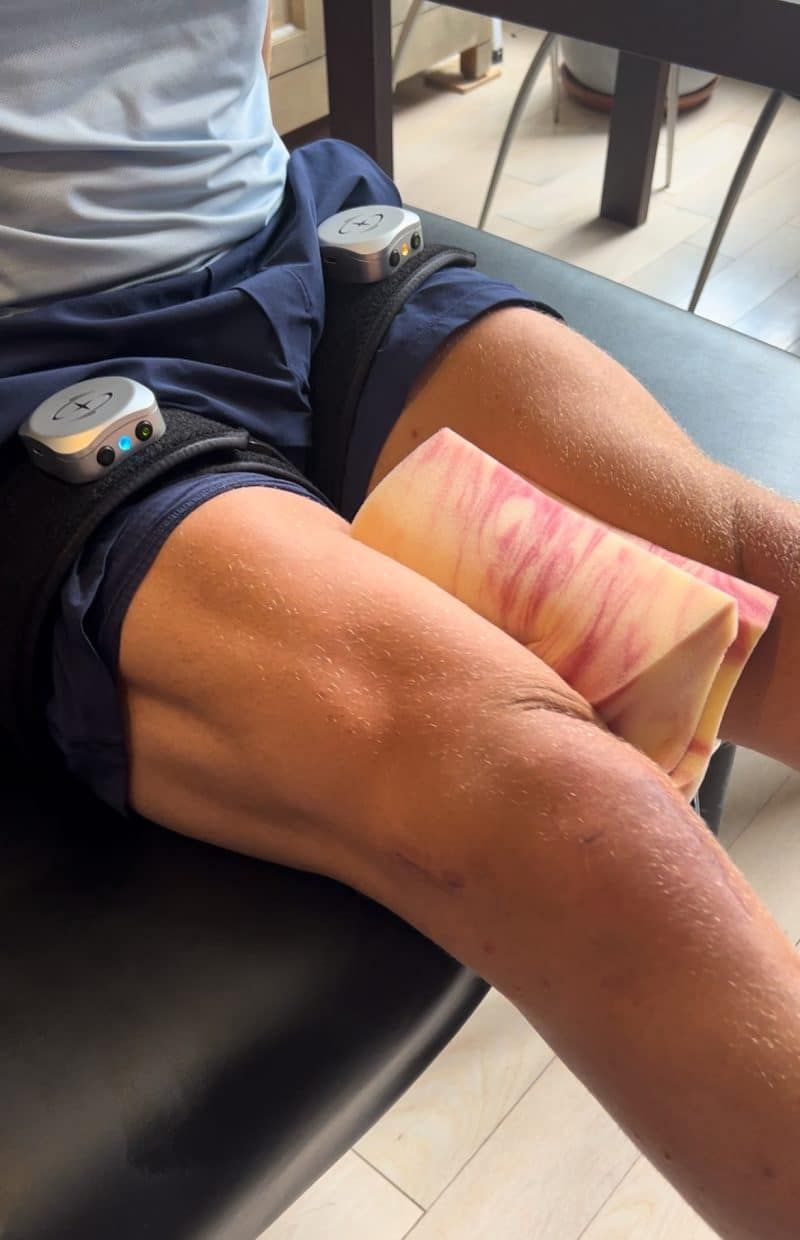
3. Blood flow restriction training (BFRT) is extremely effective in the early stages of rehabilitation. About a decade ago BFRT became more widely available for clinicians and the general population. As a result, now more evidence is emerging showing the benefit of this training for muscle mass reduction after injuries. This is simply because this type of training puts stress on the muscles through metabolic stress rather than mechanical stress (lifting weights for example). After ACL reconstruction the patient is unlikely to be able to move the knee, let alone to lift weights. BFRT will allow the patient to avoid significant loss of muscle mass from inactivity (muscle atrophy) and overall weakness, promoting muscle reactivation.
4. Training under fatigue is crucial in the late stages of rehabilitation to avoid additional injury or re-injury. This is addressed during the last stages of physical therapy, when the athlete is placed in as close to real life sport environment and stress conditions as he/she can be. It is common to hear of an athlete who has undergone and passed both physical therapy and strengthen and conditioning programs, and still ended up re-injuring the same knee or the other knee. One of the reasons for this is that these programs often don’t try to match the demands that are placed on the athlete in real life while in their sport. This necessitates intense programming in which reaching fatigue is the goal.
Fatigue, as it relates to endurance training, will test not only the athlete’s ability to sustain strength and muscle contraction, but also their ability to generate force as it relates to their neuromuscular system.
As a side note, fatigue can be stressed in the late stages of rehabilitation not only by the traditional sport specific endurance training, combined with strength and power training that puts increased mechanical stresses on the joints and muscles specifically. It can also be achieved by combining BFRT with these types of training as a way to fatigue the tissues both metabolically and mechanically.